The word ‘arthritis’ is used to describe pain, swelling, and stiffness in one or more joints. However, it is not a single condition and there more than 100 types of arthritis and related conditions. The underlying cause varies with specific types of arthritis. It can cause everlasting joint changes and the common joint symptoms may include swelling, pain, stiffness, and decreased range of motion gradually.
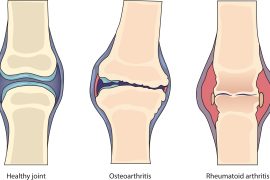
These differences may be noticeable, such as lumpy finger joints, but usually, the damage can only be detected on X-ray. Apart from joints, some types of arthritis also affect the heart, eyes, lungs, kidneys, and skin. Although there are numerous types of arthritis, the two most common ones are Osteoarthritis and Rheumatoid arthritis.
Osteoarthritis
Osteoarthritis is a chronic (long-lasting) joint condition, affecting millions of people globally. In this case, the cartilage (protective tissues covering the ends of bones forming a joint) breaks down, causing the bones within the joint to rub together. Other causes may include dislocated joints and ligament injuries.



Signs that you may have Osteoarthritis:
- Joint stiffness and soreness
- Grating sensation
- Bone spurs
- Loss of flexibility
Treatment of Osteoarthritis
A) General Management
Patients with osteoarthritis of the hand may benefit from assistive devices and instruction on techniques for joint protection; splinting (a rigid or flexible device that maintains in position a displaced or movable part) is beneficial for those with symptomatic osteoarthritis.
Patients with mild to moderate osteoarthritis of the knee or hip should participate in a regular exercise program (e.g. a supervised walking program, hydrotherapy (water cure) classes) and, if overweight, should follow a healthy and balanced diet. The use of assistive devices can improve functional status.
B) Medical Management
- Oral nonsteroidal anti-inflammatory drugs (NSAIDs) – Common NSAIDs are ibuprofen and diclofenac; painkillers.
- Topical therapies – Topical NSAIDs are applied to unbroken skin where it hurts in the form of gels, creams, sprays, or plasters.
- Intra-articular injections – A term used to define a shot delivered directly into a joint with the primary aim of relieving pain.
C) Surgical Measures
Total hip and knee replacements provide excellent symptomatic and functional improvement when the involvement of that joint severely restricts walking or causes pain at rest, particularly at night. Total Knee Replacement is one of the most common surgeries in the world with a large majority of patients going on to lead rich, happy and healthy lives. It requires a surgery of 1-2 hours followed by a hospital stay of 2-3 days.
The knee is human body’s largest joint and is made up of the lower end of the thighbone, the upper end of the shinbone and the kneecap. A knee replacement includes replacing some or all of the component surfaces of the knee joint with artificial implants. A knee replacement is performed to repair the damaged weight-bearing surfaces of the knee joint caused due to inflammatory diseases or injury. The damage overtime leads to extreme pain and can restrict joint mobility. Knee replacement is a major surgical procedure requiring hospital admission for 2 to 3 days.
Rheumatoid arthritis
Rheumatoid arthritis (RA) is an autoimmune disease; a condition in which your immune system mistakenly attacks your body. It happens when your immune system targets your joints lining. While RA affects joints on both sides of the body such as both hands or both knees, it can also affect your whole body.
Signs that you may have Rheumatoid arthritis:
- Joint pain, swelling, and tenderness
- Morning stiffness for at least 30 minutes after waking up
- More than one joint affected (hands or wrists)
- Fever



Treatment of Rheumatoid arthritis
The primary objectives in treating rheumatoid arthritis are reduction of inflammation and pain, preservation of function, and prevention of deformity. Success requires early and effective medication. Disease-modifying anti-rheumatic drugs (DMARDs) should be started as soon as the diagnosis of rheumatoid disease is certain and then adjusted with the aim of suppressing disease activity. NSAID drugs are members of a drug class that reduces pain, decreases fever, prevents blood clots, and in higher doses, decreases inflammation and provides some symptomatic relief in rheumatoid arthritis but do not prevent erosions or alter disease progression. They are not appropriate for monotherapy (therapy that uses one type of treatment) and should only be used in conjunction with DMARDs, if at all.
Possible causes of arthritis may include injury, abnormal metabolism, inheritance, infections, or immune system dysfunction. Seek immediate medical care if you have swelling or stiffness that doesn’t go away in a few days or if it becomes too painful to touch your joints. If joint pain isn’t connected to any recent injury, you must immediately consult your doctor.
It’s normal to have joint pain occasionally, but when the pain starts interfering with your daily movements, it’s time to seek medical help. The initial move is to get an accurate diagnosis of what’s causing your joint pain. You may be later referred to a rheumatologist or orthopedist (Doctors who specialize in arthritis and related conditions). During the medical examination, your doctor may ask questions related to your symptoms and medical history to assess your situation.
Although there’s no particular cure for arthritis, treatments have developed gradually. The treatment for arthritis aims at controlling pain, lessen joint damage, and enhance the quality of life. A variety of medicines and lifestyle changes can help accomplish this and protect joints from additional damage.