Welcoming a new baby into your life is a joyous occasion, but if you’ve had a C-Section, you might be wondering about the best ways to care for your scar and ensure a smooth recovery. The good news is that with the right tips and a little bit of patience, you can heal comfortably.
What are C-Section Deliveries?[1]
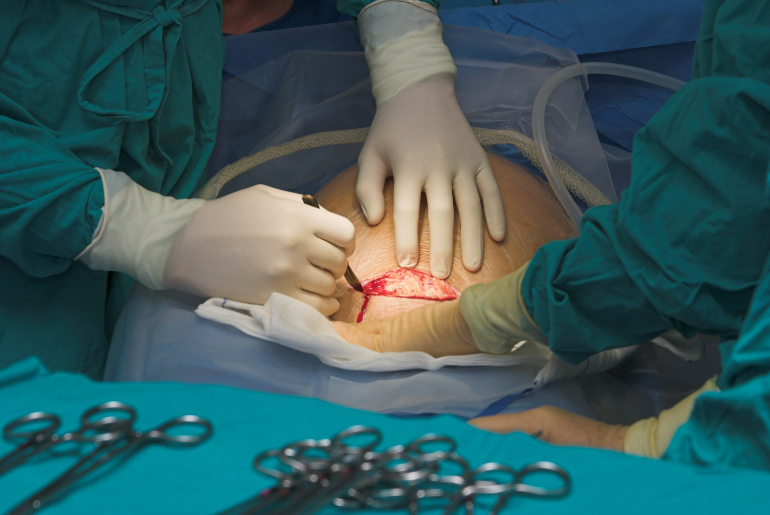
A C-Section is a surgical procedure which is used to deliver a baby through incisions. These incisions are made in the abdomen and uterus. This method is often chosen when vaginal delivery poses risks to the mother or baby or due to specific medical conditions. While C-Sections are generally safe, they require a recovery period as the body heals from the surgery.
Types of C-Section Incisions[2]
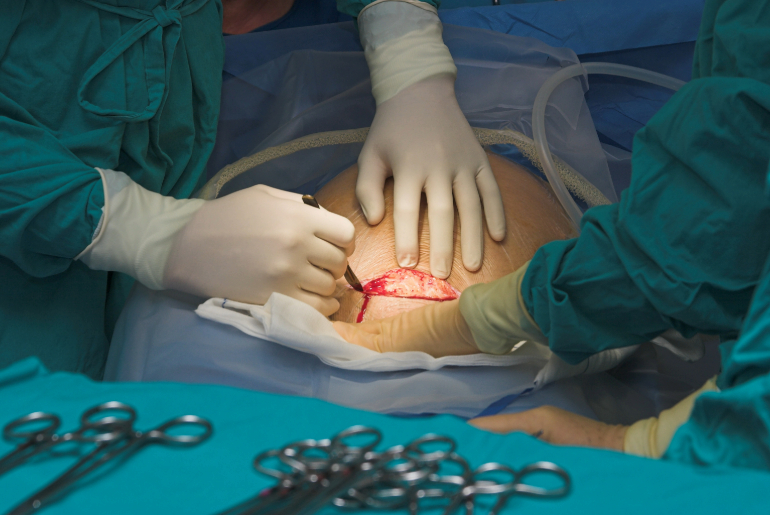
C-Section incisions can be either horizontal or vertical. The horizontal incision, also known as a bikini cut, is made just above the pubic area and is more common due to its cosmetic advantages. A vertical incision runs from the navel to the pubic area and is typically used in emergency situations.
Normal Healing Process of C-Section Incisions[2]
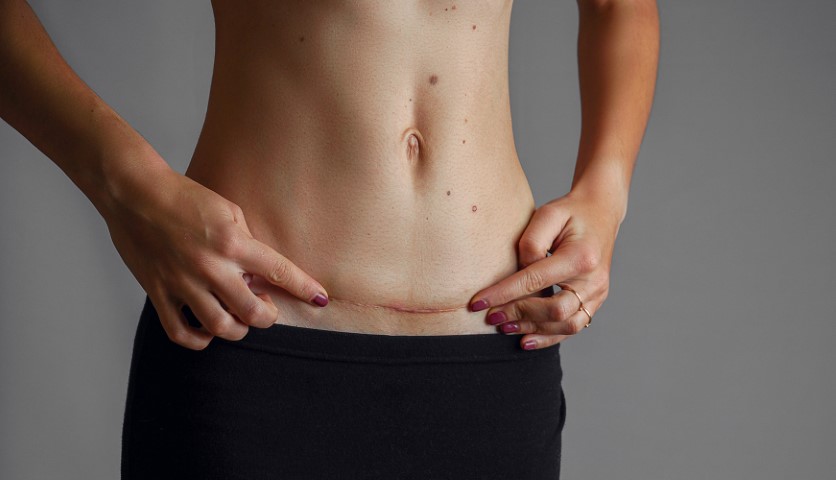
After a C-Section, the body begins the healing process immediately. It’s normal for the scar to be red and slightly raised initially, but it will gradually fade and flatten over time. Full recovery and scar maturation can take up to a year.
Immediate Post-Operative Care of C-Section Incisions[2]
- Follow Medical Advice: Your doctor will give you specific instructions on how to care for your incision. Following these instructions diligently is crucial for preventing infections and promoting healing.
- Keep the Incision Site Clean: Ensure the incision area is kept clean and dry to prevent any kind of infection. Gently clean the area with mild soap and water, and pat it dry. Absolutely avoid using harsh chemicals or scrubbing the scar.
- Signs of Infection: Watch for signs of infections such as redness, swelling, or discharge. If you notice any of these symptoms, contact your healthcare provider immediately.
- Pain Management: Your doctor may prescribe medications that are effective. Always follow your healthcare provider’s advice regarding pain relief.
Healing After C-Section[3]
- Importance of Rest: Rest is vital for healing after a C-Section. Avoid demanding activities and heavy lifting for several weeks. Allow your body the time it needs to recover.
- Gentle Movement and Walking: While rest is important, gentle movement is equally beneficial. Walking might help improve circulation and prevent blood clots. Start with short walks and gradually increase the duration as you feel comfortable.
- Maintaining a Balanced Diet: A nutritious diet rich in vitamins and minerals supports the healing process. Add plenty of fruits, vegetables, lean proteins, and whole grains in your diet.
- Drinking Water: Hydration is crucial for overall health and recovery. Drink plenty of water throughout the day to keep your body hydrated and support the healing process.
Wrapping It Up
Caring for your C-Section scar is an essential part of your postpartum recovery. Remember, every mother’s journey is unique, so be patient with yourself as you walk on the path to recovery. Embrace the healing journey, knowing that you are taking the best steps for your well-being and enjoying the precious moments with your newborn.
Reference Links:
[1] https://my.clevelandclinic.org/health/treatments/7246-cesarean-birth-C-Section
[2] https://www.webmd.com/baby/what-to-know-about-cesarean-scars
[3] https://medlineplus.gov/ency/patientinstructions/000624.htm